Since the beginning of the epidemic, almost 1.1 million Americans have died from Covid-19, a figure that you may be acquainted with. But here’s one you might not have heard of: According to one Centers for Disease Control and Prevention estimate, during the last three years, more than 300,000 extra Americans have died who would not have perished in more normal times.

Americans dying
“Excess mortality” estimates “anticipated” fatalities in a population based on historical and demographic patterns. Demographers, epidemiologists, and the rest of us may use that baseline to gauge surprises, such as a very terrible flu season or a new coronavirus creating a pandemic.Covid-19 has been mostly blamed for the country’s high excess mortality during the previous three years. However, a quarter of the total, and often a bigger percentage, has been attributed to other causes. This gap has come to be known as our excess excess mortality ,how much more and unexpected death the country has experienced during the pandemic than we have identified as a direct result of infection.
This “excess” can be calculated in several ways: According to The Economist, total excess mortality from the pandemic in the United States is 20% higher than the country’s official Covid death toll. A alternative CDC data set reveals that the figure is just around 10% higher. Other estimates range from a low of about 15% higher to nearly 50% higher. Almost all predict a “excess excess” of hundreds of thousands of deaths during the pandemic.
On real numbers, the numbers have decreased over time, as has the Covid-19 mortality toll, thanks to vaccination, “natural” immunity, and less virulent Omicron strains. However, the disparity between Covid-19 mortality and overall excess mortality has remained remarkably and perplexingly persistent.
As the C.D.C. processes death certificates slowly, recent data can be noisy. However, for more than six months, the agency calculated that total excess mortality was 50% higher than, and often nearly twice as high as, the number of official Covid-19 deaths, which we tend to regard as the age’s central public health anomaly.
Even though the pattern has persisted for three years, no one can agree on what is causing it from a medical or scientific standpoint. Instead, a few hundred thousand “unexpected” deaths may have only been loosely hypothesised to account for. Michael Osterholm, an epidemiologist at the University of Minnesota, told me, “We’ve got to figure this out. And to achieve that, you need to have the conversation that goes something like, “Wait a minute, this is bigger than people realise.”
Hypotheses
The first is disrupted supervision, which refers to how the pandemic caused people to put off getting treatment for a variety of conditions as hospitals and doctors prioritised patients with Covid-19 and diverted resources away from those with other conditions, and cancelled visits and screenings stopped new diagnoses (and therefore treatment).
A second theory concerns the indirect effects of pandemic restrictions, including not only missed medical care but also social isolation, anxiety, and unemployment, all of which can exacerbate a number of conditions, as well as possibly suicide, homicide, and even auto accidents and drug overdoses, to the extent that each deviated from historical norms.
A third theory is that Covid-19 infection causes harm to the body that, in some cases, may persist even after recovery. This harm may manifest not only as what is known as long Covid, but also in other ways, such as by interfering with the operation of different organ systems. (One area of research that has received particular attention is damage to the cardiovascular system.) The Yale immunobiologist Akiko Iwasaki told me, “We still don’t truly understand the whole spectrum and breadth of illness yet. We continue to learn.
The risk of these “post-acute sequelae” with reinfection, rather than just initial infection, has been the subject of papers exploring a different theory over the past year, which has also caused considerable concern. Nearly all of the several specialists I spoke with regarding these articles underlined their flaws, most notably the fact that their authors were only interested in the health consequences of patients who had seen a doctor while feeling sick.
They informed me that, if the effect size was real, it was almost certainly much smaller than the write-ups suggest. However, almost every expert was careful to add that, given the same circumstances, a reinfection was in fact bad for you, that you’d want to avoid them especially if you weren’t in great health, and that in certain circumstances, a reinfection could undoubtedly be a factor in a patient’s death from causes other than the classic Covid pneumonia.
Another theory is that in certain people with COVID infection, immunological function is permanently damaged. Although there has been a lot of pushback and contestation against and contextualising for narratives of significant and widespread immunological dysfunction, papers have been published here as well that trace immunological effects.
Although I have presented each of these theories separately, they are still intertwined. Beyond the heartache it causes, one of the many lessons I’ve learned from the pandemic is how much more complicated and perplexing disease severity and death are. I’ve also learned how unpredictable illness progression can be, how oversimplified it can feel to attribute a single cause of death, and how random individual outcomes can seem.
Despite how complicated and nuanced so many of the cases ended up being, we still wanted the narratives we drew from the pandemic to be clear and understandable. What would you attribute the death of a person with terminal cancer if they had a Covid-19 infection that caused them to pass away six months earlier than they might have otherwise? What about those who developed worse Alzheimer’s, obesity, or anxiety in isolation before passing away from a Covid infection? Or those who merely hadn’t undergone Covid testing?
If two, three, or five factors contributed to a specific death, how exactly do you assign blame? And should we refer to a death as occurring “from” Covid-19 if it was the fifth contributing factor yet the death would not have occurred without the infection?
Given that fewer patients are dying from Covid pneumonia now than they did at the beginning of the pandemic, and that Covid is increasingly listed as a secondary or contributing cause on death certificates, these are difficult questions, and they occasionally spark tense discussions about whether the nation as a whole may be overestimating Covid-19 mortality. Two fact-checks of a Washington Post column that sparked some recent controversy were recently published by the C.D.C. But where are the country’s relatively high numbers of deaths actually coming from if we are purposefully overcounting pandemic mortality by attributing deaths to Covid rather than other causes?
Excess mortality calculations have limitations because it is difficult to predict the future more than a year or two out even with good data and accurate modelling. While the C.D.C., which has not always handled its data as effectively as some European nations, utilises data going back to 2013, the majority of the modelling through the pandemic has been done with data from 2015 to 2019, meaning part of it is already eight years out of date.
Francois Balloux, a computational biologist at University College London, cautioned, “We have to be a bit careful,” highlighting the uncertainties in the models, the variations among them, and the ways that minor changes to demographic assumptions can significantly alter expected mortality projections and, consequently, excess mortality findings. Despite these drawbacks, one of the greatest strengths of this paradigm is that it enables you to step back, out of the minutiae of one argument or another, and see the broad picture. And regardless of the model, the overall picture is fairly obvious.
Each of the five theories I listed above has a reasonable chance of explaining a portion of this phenomenon, this excess excess, which manifests itself in other nations on various scales.
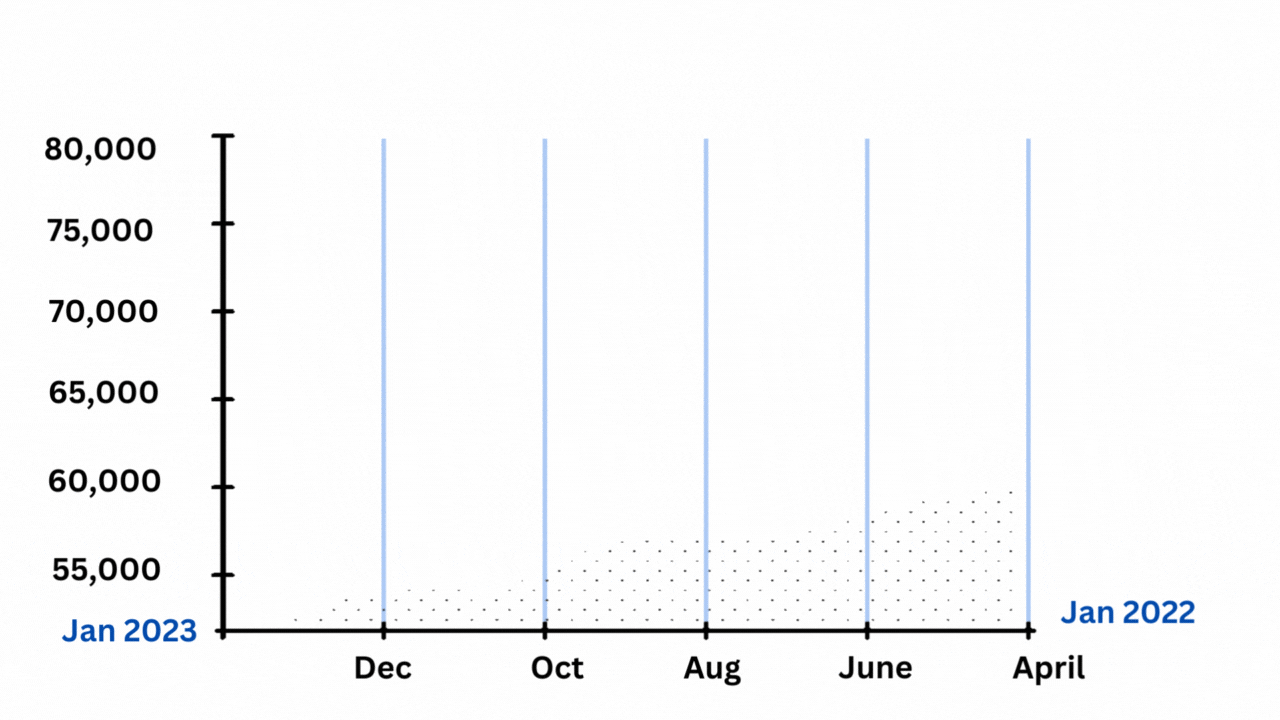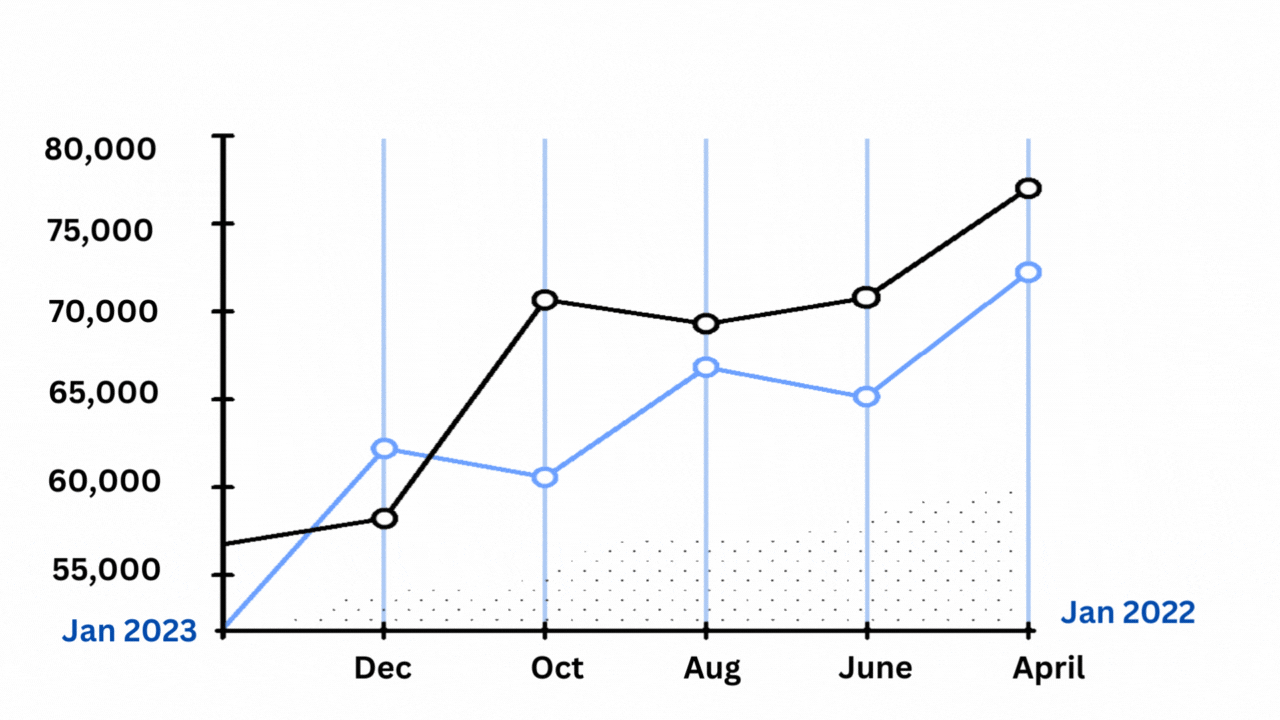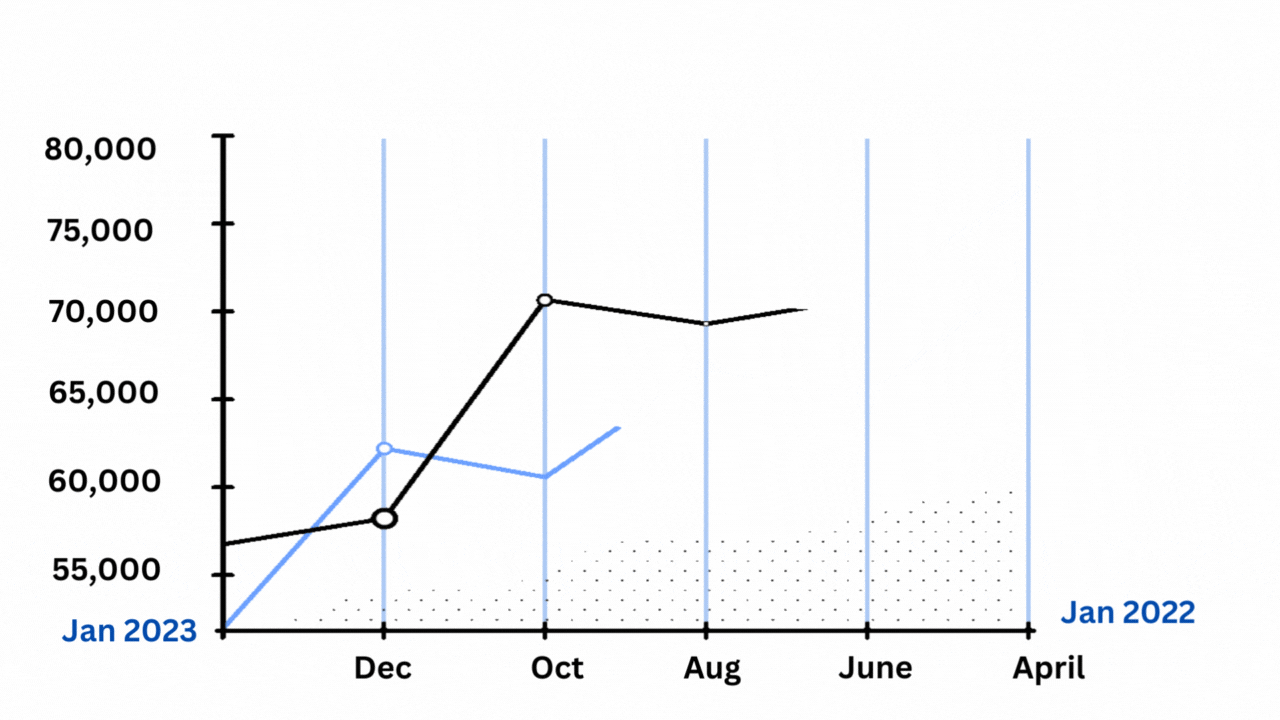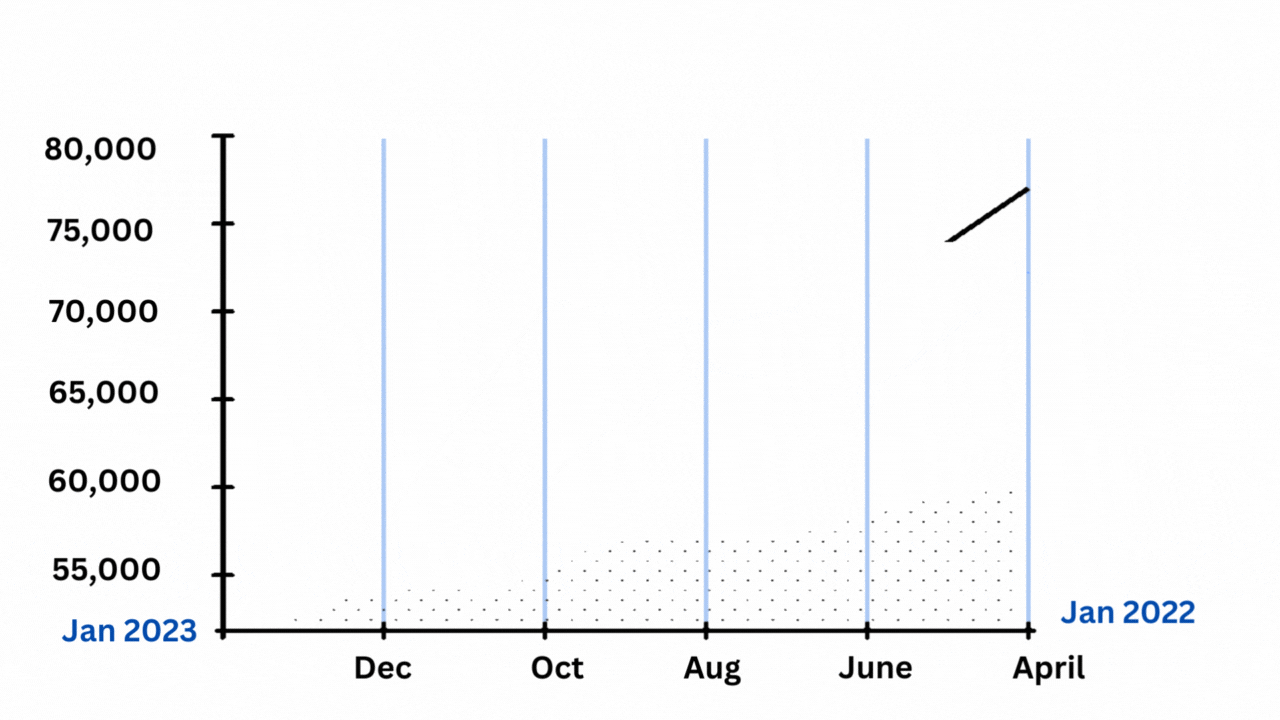
However, there are reasons to doubt that they offer a complete explanation, even when considered all at once. The excess mortality curve’s shape, which matches the official Covid-19 death chart so closely that it appears to be high- and low-end estimates of the same phenomenon rather than multiple distinct stories, is another important factor.
Excess deaths and Covid-19 deaths have been strongly correlated.
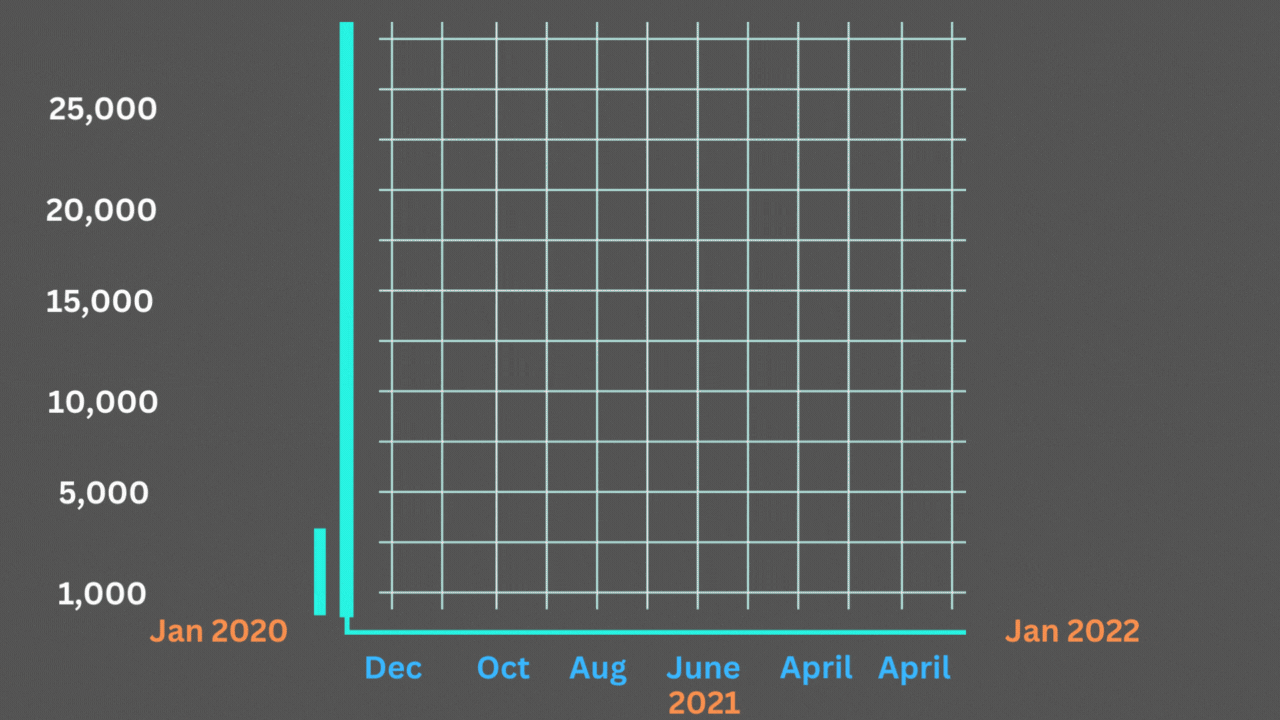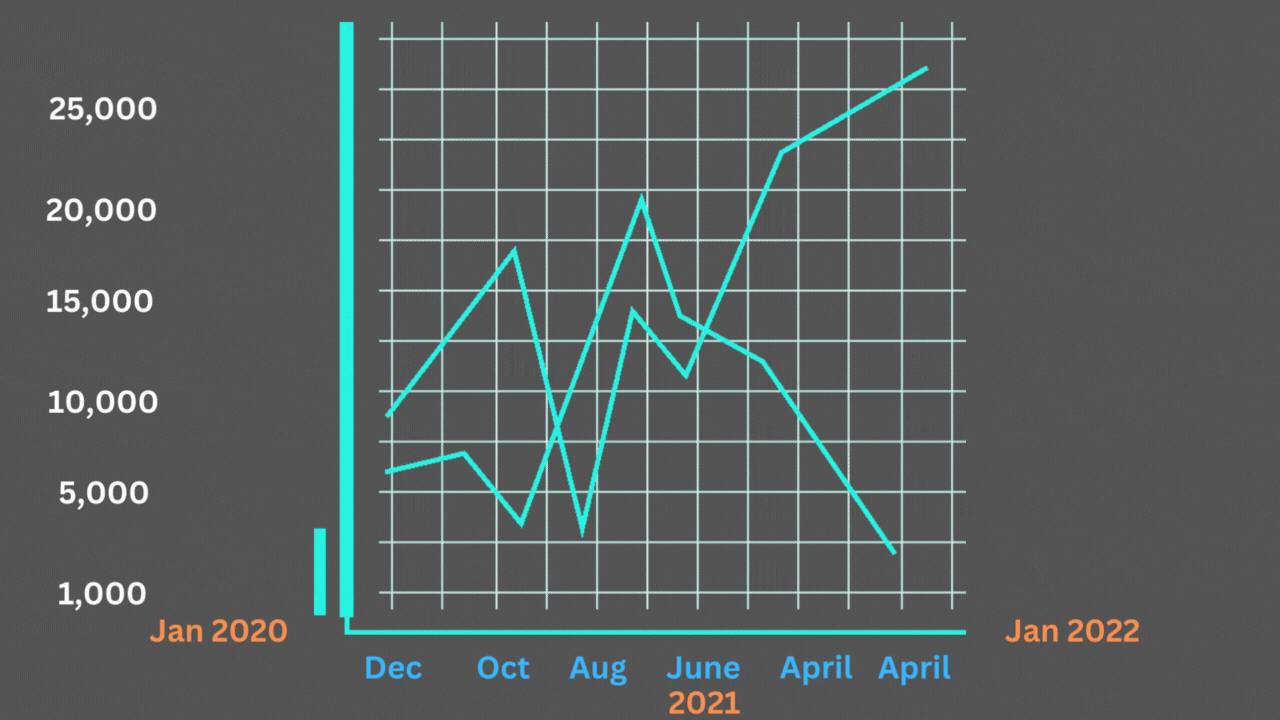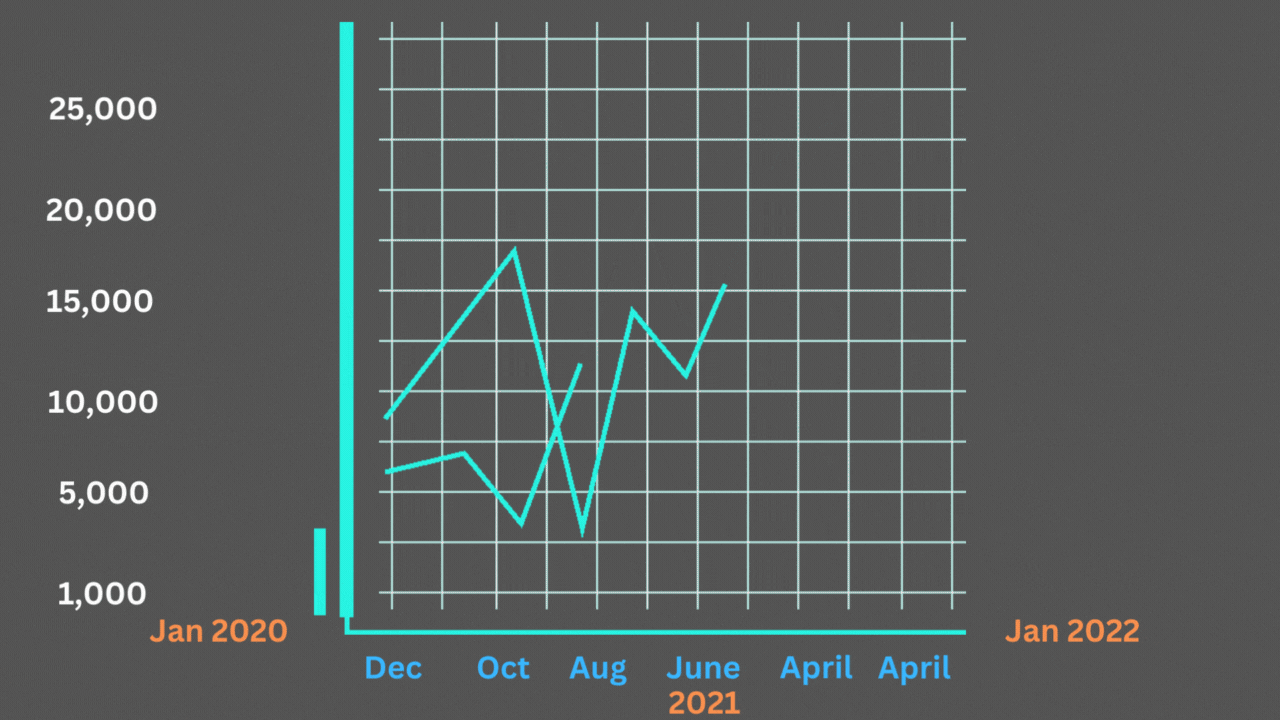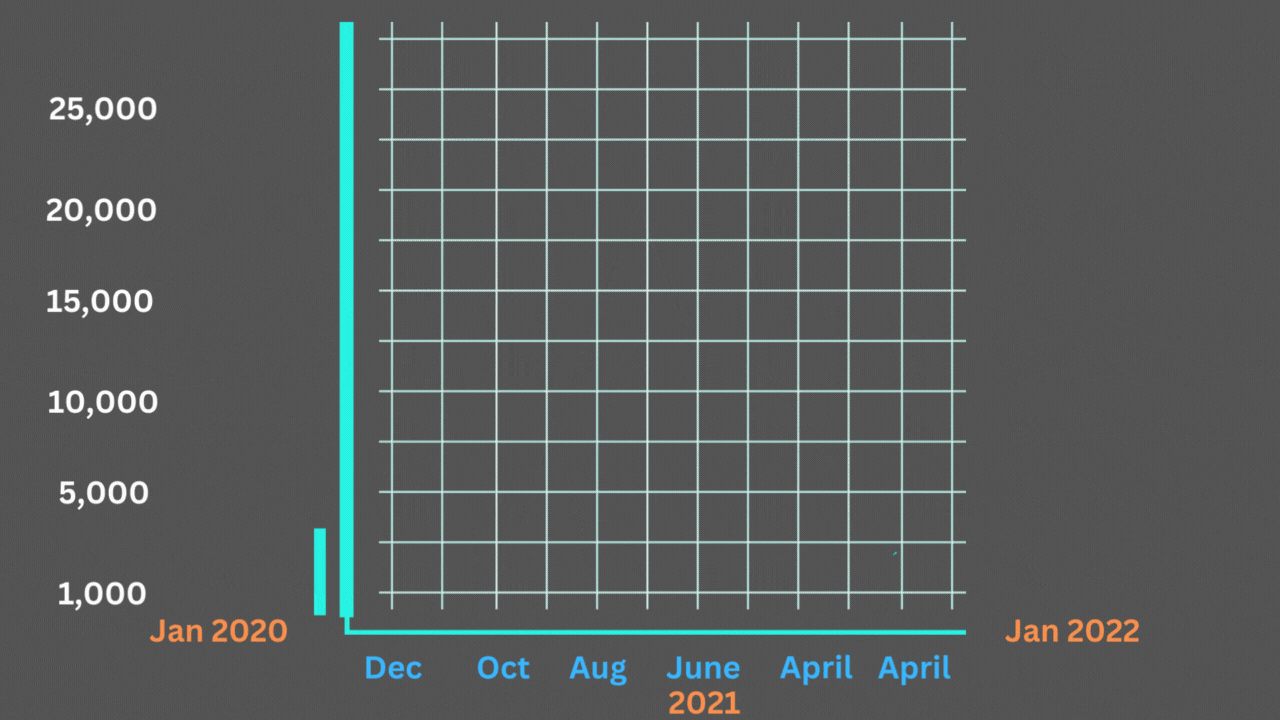
The Economist’s graphics may be viewed here. The chart above is based on the lower-end estimates of extra fatalities provided by the C.D.C. Each excess peak is matched by a Covid-19 high, as Harvard’s Jeremy Faust and Benjy Renton have noted in a series of postings after looking at their own excess-mortality statistics. With each individual trough, the same holds true.
This pattern is not entirely explained by the traditional theories. The fact that care resumed with substantially less interruption after 2020 is likely to bias the impact if the extra excess was mostly a result of delayed care. Since many diseases take time to progress to their final stages, early pandemic delays in diagnosis and treatment may still be having an impact today.
It’s not difficult to explain how undiagnosed heart disease and postponed cancer treatments contribute significantly to overall mortality rates, but it’s much more challenging to explain why that effect would scale so neatly with waves of official Covid deaths. One C.D.C. database indicates that there were only about 28,000 “above average” cancer deaths during the full pandemic, despite the fact that cancer is the illness that is likely to come to mind when thinking about these risks.
That represents a tiny portion of the excess mortality and an even smaller portion of the more than 1.5 million cancer-related deaths in the United States since 2020. (The C.D.C. places a significantly bigger portion of the extra excess attributable to dementia, Alzheimer’s, and cardiovascular and circulatory disorders.)
Overdoses, homicides, suicides, and auto accidents have all increased during the pandemic, but not to the extent necessary to account for the entire excess mortality. According to Faust, these deaths have only contributed to 5% of excess mortality during periods of high Covid-19 spread and up to 25% of excess mortality during periods of low Covid mortality. This is due to the fact that although the number of fatalities from those causes increased in the summer of 2020, they have essentially remained flat ever since. (They are also concentrated in the young, whereas the official Covid-19 toll has an old-skewing due to excess.)
We should anticipate a rise in non-Covid excess fatalities at some point after each specific wave of infection, possibly a few weeks or perhaps a few months later, if protracted Covid or post-acute sequelae were the primary culprits. (If vaccination risk were a factor, it might produce the same pattern; however, the curves do not support this.) As with immune dysfunction and the risk of reinfection, we might anticipate that as the total number of infections rises over time, so will the share of non-Covid excess mortality. Although there were more American infections in 2022 than in either of the two years prior, the excess excess was actually less than in 2020 in terms of absolute numbers.
Faust thinks he has at least a partial solution to the riddle: a major portion of the excess excess mortality is made up of Covid-19 fatalities that happened at home but were not properly reported or registered as a result.
According to the tale he tells, a grandmother or grandfather is discovered unresponsive at home; an ambulance is called; the paramedics pronounce the person dead; the grandparent wasn’t recently tested for COVID but had been feeling unwell for a few days, according to the relatives, who themselves recently had COVID; the deceased also had heart disease, and so that is recorded as the cause of death.
Theoretically, in a hospital setting, doctors might add Covid to a death certificate in more cases than necessary since all patients will have been tested and many will be positive as a result of in-hospital transmission. However, in an at-home situation, you cannot link a fatality to Covid-19 without a positive test, suggesting that a sizable portion of such deaths may go unrecognised.
Throughout the pandemic, Covid-19 has been blamed for about 20% of in-hospital deaths compared to a meagre 2% of deaths at home. The Covid death toll would increase slightly but the excess excess gap would almost entirely disappear if you roughly tripled the share of at-home deaths attributed to Covid, which is still significantly less than the share in hospitals. Additionally, you actually overestimate the difference if you adjust it to reflect the percentage of fatalities attributable to Covid in settings other than residences, such as hospitals, outpatient clinics, and nursing homes.
According to Faust’s own study, the excess excess is more when there is less testing and lower when there is more testing. He predicted that eventually it would be discovered that between 80,000 and 90 percent of the 200,000 to 300,000 additional deaths were caused solely by Covid.
You could debate whether infection was the main cause of these deaths or just one of many contributing factors. But according to Faust, the Covid waves that coincided with them are the reason we have so many. Although it may be superior to that in other nations, our public health surveillance is definitely far from ideal.
The number of deaths among Americans is still more than anticipated, thus at some time, the country may need to raise its estimation of annual deaths by at least a small amount. Beyond vaccination, the nation abandoned the majority of mitigation measures a long time ago. (And even there, the uptake of boosters has been very low.) Whatever the intuitive implications of these questions, it’s unlikely that, however they are resolved, all that much about pandemic policy will change. The Biden administration announced this week that the Covid-19 public health emergency would end in May.
But somehow, depending on how we interpret that excess excess, the story of the pandemic appears to be quite different. The direct mortality toll from Covid-19 in the United States would increase to about 1.5 million if the majority of those tens of thousands of extra fatalities were attributed to Covid infection, which is probably the simplest, Occam’s razor explanation. It implies some degree of pandemic overreach if we attribute it to delayed care and social isolation, and it suggests the possibility of an ongoing public health burden if we attribute it to long Covid and post-acute sequelae. It would be wonderful to know for sure.